A historic meeting between chiropractic and Make America Healthy Again (MAHA) leadership took place on March 10th, 2026, in Washington, D.C., featuring representatives from chiropractic national organizations, professional associations and policy principals. The collective goal: advancing the role of chiropractic in improving the health of Americans. Meeting participants focused on long-standing issues that have affected the chiropractic profession for decades, including access to care, reimbursement parity, and ensuring DCs have an appropriate role in national health policy discussions.
| Digital ExclusivePlantar Plate Injuries: Conservative Management
- The plantar plates play a key role in protecting the metatarsal heads from trauma and stabilizing the toes during the propulsive phase of gait.
- Despite the strength of stabilizing ligaments, the plantar plate is frequently injured and the plate beneath the second metatarsal head is especially prone to injury.
- Effective conservative management of a plantar plate injury involves minimizing tensile strain on the plantar plate during the healing process and addressing the biomechanical factors that contributed to its occurrence.
The plantar plates are a series of fibrocartilaginous disks located beneath the lesser metatarsal heads. These plates play a key role in protecting the metatarsal heads from trauma and stabilizing the toes during the propulsive phase of gait.
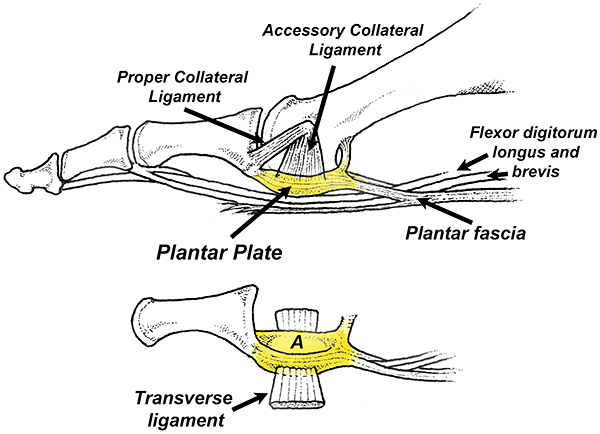
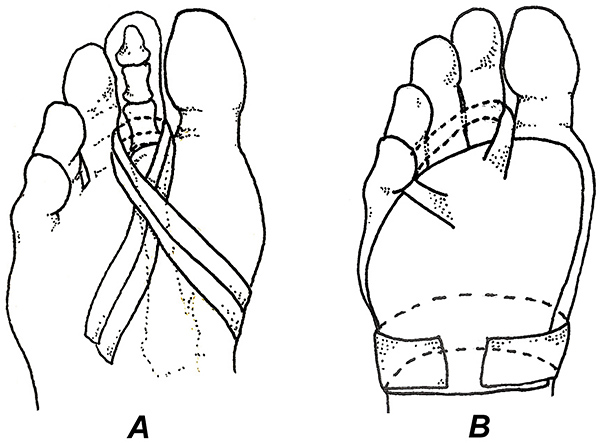
Anatomically, the plantar plates originate from the distal shafts of the lesser metatarsals and insert directly onto the proximal phalanges. Each plantar plate receives powerful attachments from the accessory collateral and transverse ligaments, and the longitudinal branches of the plantar fascia. (Fig. 1)
Importantly, the plantar plate does not attach uniformly to the proximal phalanx. Instead, its major attachments are on the medial and lateral sides of the base of the phalanx. This dual attachment allows the plantar plate to function like a cushioned sling (Fig. 1A) that protects and cradles the metatarsal head as it rotates and slides in response to weight-bearing activities.
Biomechanical Factors
Despite the strength of these stabilizing ligaments, the plantar plate is frequently injured and the plate beneath the second metatarsal head is especially prone to injury. While the plantar plates can be injured secondary to trauma (usually a hyperdorsiflexion injury), there are various anatomical / biomechanical factors that increase the likelihood of injury.
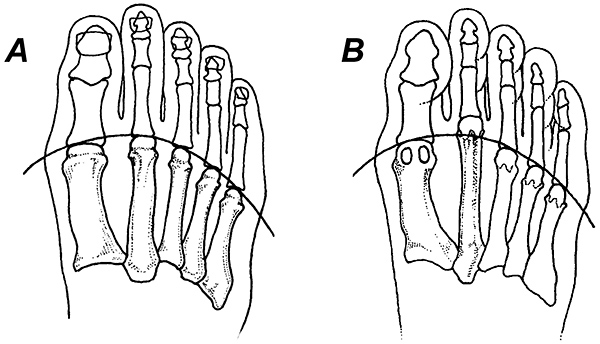
The most frequent biomechanical cause for plantar plate injury is an elongated second metatarsal.(Fig. 2) Other biomechanical factors frequently associated with plantar plate injuries include hypermobile first rays, Morton’s foot structure and hammer toe deformities.1
Plantar plate injuries can also be the result of limited ankle motion, as isolated contracture of the gastrocnemius produces an early heel lift that greatly increases the risk of forefoot injury. DiGiovanni, et al.,2 demonstrated that people with less than 5 degrees of ankle dorsiflexion are three times more likely to complain of pain in the forefoot / midfoot.
An Overlooked Contributor?
Though rarely discussed as a possible etiological factor, toe weakness results in increased stress being placed on the central plantar plates. As demonstrated by Ferris, et al.,3 the long toe muscles distribute pressure away from the second and third metatarsals onto the tips of the toes. Additionally, a strong peroneus longus can offload the central forefoot by transferring force to the first metatarsal head, which is twice as wide and four times as strong as the neighboring lesser metatarsals.
Symptoms / Diagnosis
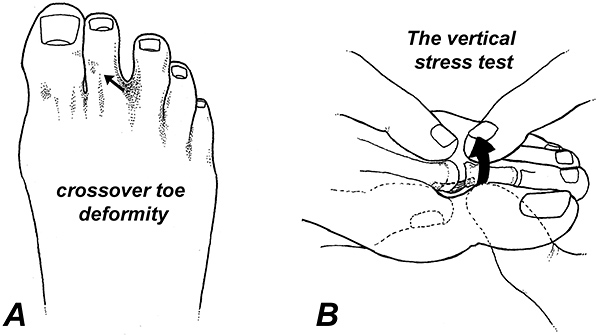
Initial symptoms associated with plantar plate injuries include a mild aching beneath the metatarsal heads, which is often reported as a “bruised feeling.” As the plantar plate injury worsens, the characteristic “crossover toe deformity” develops, and the involved toe becomes adducted and often hammered. (Arrow in Fig. 3A)
The most important diagnostic test confirming the presence of a plantar plate tear is the vertical stress test (Fig. 3B), which has a sensitivity of 80.6% and a specificity of 99.8% for diagnosing plantar plate injuries.4
Conservative Management
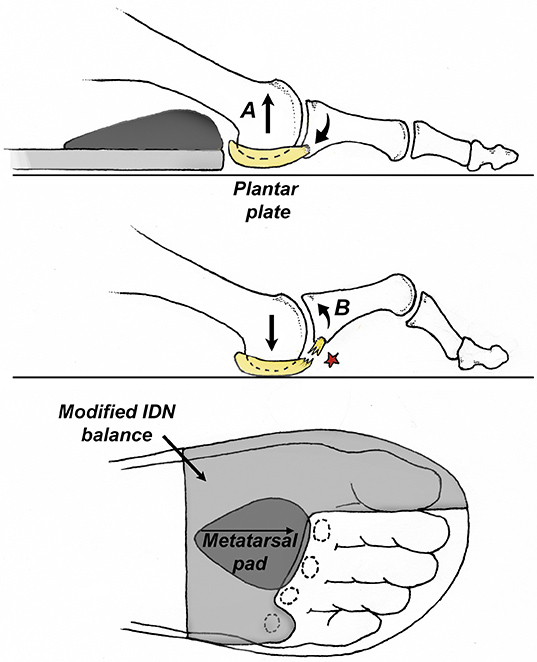
Effective conservative management of a plantar plate injury involves minimizing tensile strain on the plantar plate during the healing process and addressing the biomechanical factors that contributed to its occurrence. The easiest way to reduce tension on the plantar plate is to incorporate a metatarsal pad and add a modified EVA balance as illustrated in Figure 4.
The metatarsal pad elevates the neck of the metatarsal, distributing pressure away from the head, while the balance offloads the central metatarsal heads by transferring pressure to the medial forefoot and great toe. By lifting the metatarsal heads upward with the metatarsal pad and balance, the base of the toe moves down slightly, which approximates the plantar plate with its insertion.
The metatarsal pad and balance should be worn in shoes possessing exaggerated toe springs, as an elevated toe spring reduces upward motion of the toes while walking and running.5
Individuals with substantially hammered toes should consider using the taping techniques illustrated in Figure 5. Although effective at limiting upward motion of the proximal phalanx, these taping procedures are often relatively uncomfortable, and it is important to use a flexible tape and get feedback regarding tape placement. Taping is almost always more effective when combined with metatarsal pads.6
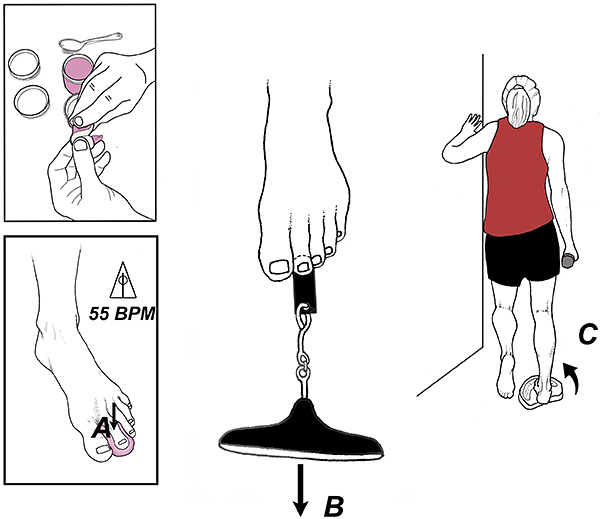
Within the first week or so following injury, gentle foot/ankle strengthening exercises should be encouraged. While often overlooked, it is essential to address the toe affected by the plantar plate tear, as this toe frequently exhibits significant weakness due to the cortical inhibition that is commonly linked with chronic pain. Studies show that exercising to the beat of a metronome, especially during isometric contractions, can reduce cortical inhibition and improve motor output.7-8
The exercise illustrated in Figure 6A typically restores toe strength in 4-6 weeks and strength gains can be monitored using the paper grip test beneath the involved toe. (Fig. 6B) This exercise should be included in a comprehensive exercise routine that targets all of the intrinsic and extrinsic foot and ankle muscles. Exercising the peroneus longus is especially important, as this muscle can offload a damaged plantar plate by stabilizing the first metatarsal head. (Fig. 6C)
Last, but not least, isolated contracture of the medial gastrocnemius must be addressed, as the premature heel lift associated with this condition drives the central forefoot into the ground perpetuating the plantar plate injury. The best outcomes occur when holding stretches for a minimum of 45 seconds and repeating these stretches at least five times per day.9
Gait changes should also be recommended, and patients with plantar plate injuries should be encouraged to walk and run with shorter stride lengths until the injury has healed. They should also practice forcefully pushing down with their big toes during the propulsive phase of gait for at least five minutes daily, as this creates a motor engram that teaches the toe muscles to offload the central forefoot.
Should conservative treatment fail, various surgical options exist, including the Weil osteotomy and/or direct reconstruction of the plantar plate. Although these procedures have proven efficacy and good long-term outcomes, they are rarely necessary, as the vast majority of people with plantar plate injuries respond to conservative care.
References
- Jastifer J, Doty J, Claassen L. Current concepts in the treatment of metatarsophalangeal joint instability of the lesser toes: review, surgical technique, and early outcomes. Fuß & Sprunggelenk, 2017;15(4):225-236.
- DiGiovanni C, et al. Isolated gastrocnemius tightness. JBJS, 2002;84(6):962-970.
- Ferris L, Sharkey N, Smith T, et al. Influence of extrinsic plantar flexors on forefoot loading during heel rise. Foot Ankle, 1995;16:464-473.
- Klein E, Weil L, Weil L, et al. Clinical examination of plantar plate abnormality: a diagnostic perspective. Foot Ankle Int, 2013;34(6):800-4.
- Sichting F, Holowka N, Hansen O, Lieberman D. Effect of the upward curvature of toe springs on walking biomechanics in humans. Sci Rep, 2020 Sep 17;10(1):14643.
- Ruiz-Ramos M, Orejana-García Á, Vives-Merino I, et al. Effectiveness of the Fixtoe Device® in plantar pressure reduction: a preliminary study. BMC Musculoskel Disord, 2022 May 19;23(1):475.
- Rio E, Kidgell D, Moseley G, et al. Tendon neuroplastic training: changing the way we think about tendon rehabilitation: a narrative review. British J Sp Med, 2016;50:209-215.
- Siddique U, Rahman S, Frazer A, et al. Task-dependent modulation of corticospinal excitability and inhibition following strength training. J Electromyogr Kinesiol, 2020,52,102411.
- Panidi I, Bogdanis GC, Terzis G, et al. Muscle architectural and functional adaptations following 12-weeks of stretching in adolescent female athletes. Front Physiol, 2021 Jul 16;12:701338.



