The proposed merger of the National Board of Chiropractic Examiners and Federation of Chiropractic Licensing Boards was approved by NBCE delegates and FCLB members at their respective annual meetings, held jointly in Atlanta, Ga., this year. Per the new bylaws, the new entity takes the NBCE name, with FCLB continuing as a department within NBCE. The federation will continue to enjoy Board of Directors representation on what will be a single, expanded board.
| Digital ExclusiveTreating Sciatica: Are You Misdiagnosing the Cause?
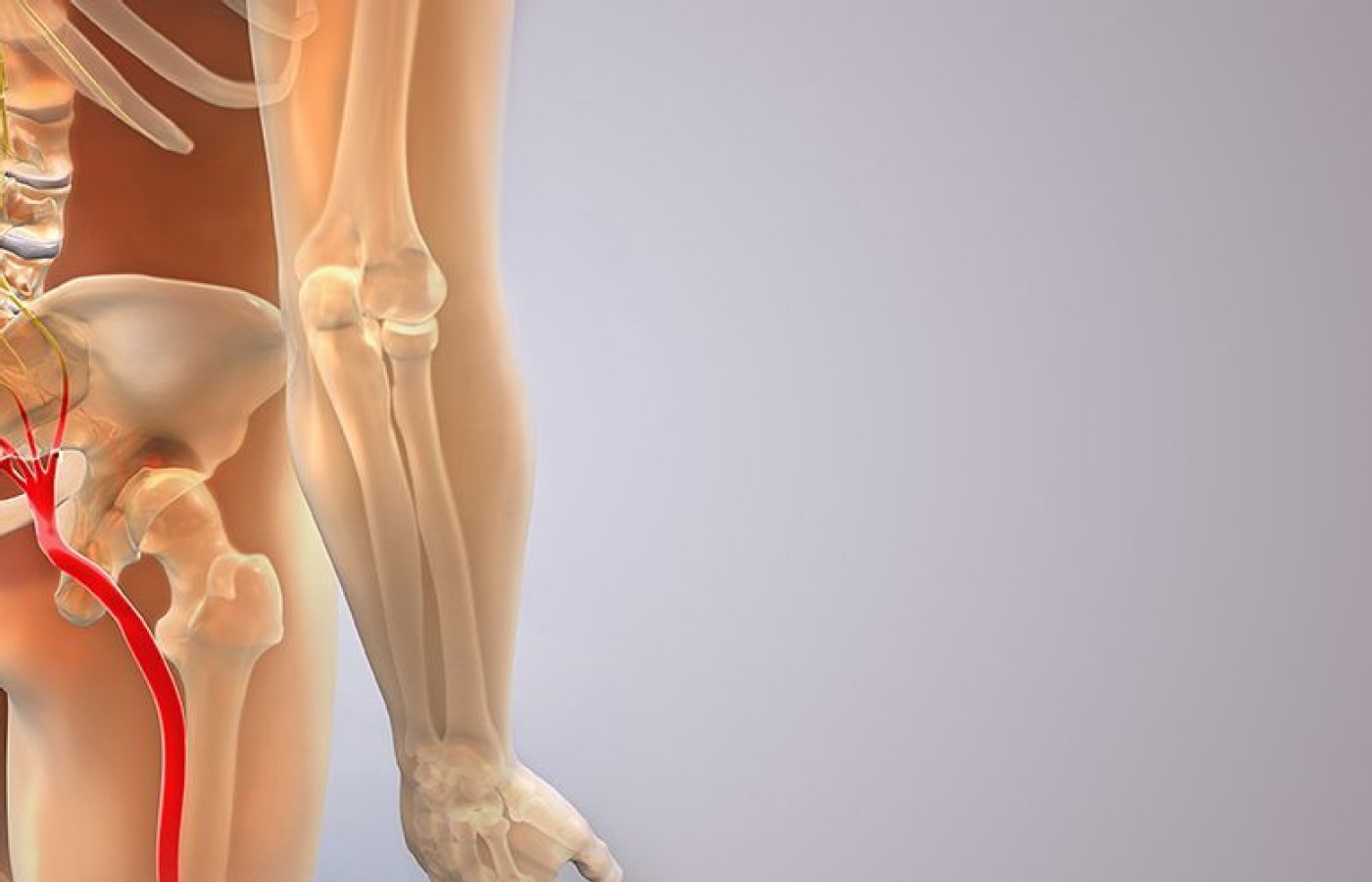
Pain down the back of the leg, the kind that settles anywhere from the buttock to the calf, is more than a disc herniation irritating the L5 nerve root. In fact, the sciatic nerve is composed of fibers from the L4, L5, S1, S2 and S3 nerve roots, which join together just above the sciatic notch in the pelvis. Therefore, to condense sciatica to an L5 nerve root irritation is too simplistic.
The classic lumbar disc lesion will have a positive straight-leg raise (SLR) for low back and/or leg pain under 30 degrees, and will be provoked by passive foot dorsiflexion on the symptomatic side. Additional provocative maneuvers to the SLR include adduction with internal rotation of the leg, seated SLR, and the slump test. These sciatic conditions are generally acute and fairly easy to diagnose.
Clinical Tip: To screen for radiculopathy versus radiculitis, look for muscle weakness in the distal distribution of the sciatic nerve. Simply test for weakness in the extensor hallucis longus (great toe extension, L5 nerve root), posterior tibial (foot inversion with plantar flexion, L4 nerve root) and peroneal (foot eversion, S1 nerve root) muscles. Weakness indicates radiculopathy of the respective nerve root.
Differential Screening
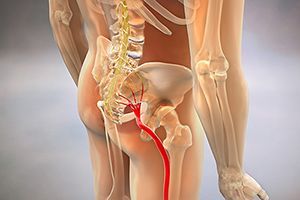
However, as the sciatic patient transitions out of the acute phase, the pain often isolates into the buttock or leg. The SLR in this phase is restricted by "tightness" more than pain; and while still limited, it is greater than 30 degrees. Provocative maneuvers can still aggravate the buttock or leg symptoms.
In addition to nerve root tension tests such as the SLR, when assessing the sciatic patient it is also important to check the mechanics of the acetabular joint and its corresponding soft tissues. Loss of acetabular joint play and hip capsule tightness can both limit SLR and lumbar spine flexion. These dysfunctions may have been predisposing to the acute sciatic condition or may be residuals from the inflammatory cascade that occurred throughout the region from the initial injury. Be sure to assess the hip and its myofascial components as part of your sciatica workup.
Clinical Tip: To determine if the SLR is limited by acetabular joint play, compare it to hip flexion with the knee bent at 90 degrees in the supine position. If the amount of hip flexion during the SLR is equivalent to the hip flexion with the knee bent at 90 degrees, the limiting variable is the hip, not nerve root tension.
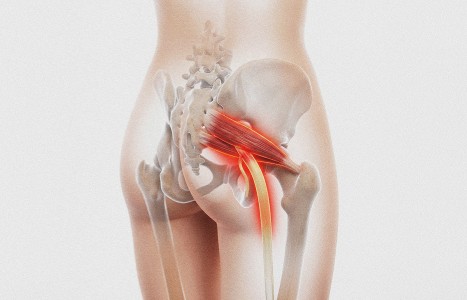
Inflammation creates a release of pro-inflammatory cytokines in the soft tissues adjacent to the sciatica nerve. This leads to increased fibroblastic activity and loss of its ability to glide between myofascial layers. When this occurs in the buttock, it appears as a piriformis syndrome; when it occurs in the upper leg, it feels like a tight, "pulled" hamstring.
Sitting fuels this process because it creates a direct pressure on the sciatic nerve in the buttocks and hamstrings, as well as increasing the load on the lumbar discs.
Clinical Tip: Piriformis syndrome, an entrapment syndrome of the sciatic nerve as it passes by or though the piriformis muscle, will be abated by external hip rotation in the 90/90 position. Statistically, it is the underlying cause of low back pain and/or sciatica only 6 percent of the time.
Nerve Flossing
"Doc, there is a dull ache right in the back of my leg, and it is worse when I sit" is a common statement we have all heard. In addition to sciatic neuritis or piriformis syndrome, this may be a tethering of the sciatic nerve between the hamstring due to the fibroblast activity mentioned above.
Regardless, restoration of physiologic nerve gliding needs to be restored. Effective techniques include manual myofascial release and neuromobilization (nerve flossing). Remember, nerves do not tolerate stretching; the intent with these techniques to promote nerve gliding between adjacent soft tissues.
Clinical Tip: For the patient with mid- to upper-posterior thigh pain that is not increased with provocative maneuvers, consider hamstring tightness. If the symptoms are lower thigh or behind the knee, consider a loss of nerve gliding as the issue.
Sciatic nerve flossing is easy to incorporate into your current treatment plan for sciatica. "Flossing" implies the nerve is encouraged to glide by pulling on the ends. One technique is while the patient is sitting: have them extend the symptomatic leg and rest it on the ground in a comfortable position.
Then instruct the patient to actively move their foot into full dorsiflexion while actively extending their head and neck, followed by full plantar flexion while the head and neck move into full flexion. Slowly repeat the full motion continuously for 10-15 repetitions or until tension releases. Be sure any buttock or leg symptoms do not increase.
Clinical Tip: An indicator for sciatic nerve gliding is to evaluate standing lumbar flexion and observe for back or leg symptoms. Then, with the patient in that position, passively extend their neck. If the leg or back pain reduces, nerve flossing techniques would be helpful.
PNF Treatment
Sitting is the new smoking and raises havoc on the muscular balance in the lumbopelvic complex. The hip flexors become shortened, hamstrings tighten and the gluteals become weak. These length-tension relationships need to be assessed and corrected in sciatic patients, adding another layer of treatment.
At a minimum, include proprioceptive neuromuscular facilitation (contract, relax, stretch) to the tight and short muscles and gluteal strengthening (bridges, curtsey squats, hip extensions) into your treatment regimen.
Chiropractic Adjustments
While nerve flossing and soft-tissue management are important in treating sciatica, the significance of assessing and treating the lumbar spine and sacroiliac joints with adjustments is essential. There are many techniques that are effective for the region; evaluate for pathomechanics and adjust accordingly. If you need to add additional chiropractic techniques for the lumbopelvic-hip complex to your CMT toolbox, take a hands-on continuing-education course.
Clinical Pearls
Sciatica can be challenging for the clinician as well as the patient. The chiropractic multimodal approach begins with CMT of the lumbar spine, SI and hips; followed by correction of acetbular capsular tightness, myofascial restrictions and muscular imbalances. Adding nerve flossing as indicated to reduce tension along the track of the sciatic nerve is another tool to get better outcomes.
Resources
- Jeanbart K, Tanner-Bräm C. Mobilization of the neurodynamic system using proprioceptive neuromuscular facilitation decreases pain and increases mobility in lower extremities and spine - a case report. J Bodyw Mov Ther, 2021 Jul;27:682-691.
- Gunn LJ, Stewart JC, Morgan B, et al. Instrument-assisted soft tissue mobilization and proprioceptive neuromuscular facilitation techniques improve hamstring flexibility better than static stretching alone: a randomized clinical trial. J Man Manip Ther, 2019 Feb;27(1):15-23.
- Liebenson C. Rehabilitation of the Spine. Philadelphia, PA: Lippincott Williams and Wilkins, 2007.