A historic meeting between chiropractic and Make America Healthy Again (MAHA) leadership took place on March 10th, 2026, in Washington, D.C., featuring representatives from chiropractic national organizations, professional associations and policy principals. The collective goal: advancing the role of chiropractic in improving the health of Americans. Meeting participants focused on long-standing issues that have affected the chiropractic profession for decades, including access to care, reimbursement parity, and ensuring DCs have an appropriate role in national health policy discussions.
| Digital ExclusiveFrom Pain Scores to Performance Metrics
- Pain intensity correlates poorly with tissue health, functional capacity, and long-term disability, particularly in chronic and recurrent musculoskeletal conditions.
- Patients may present with pain, but what they fear losing is function. Pain is an early metric. Performance defines recovery.
- By measuring performance and not just pain, chiropractors align with value-based care models while delivering outcomes patients actually care about.
Pain has become the dominant language of musculoskeletal healthcare. Numeric pain-rating scales and symptom reports are routinely used as primary indicators of clinical success. But while pain reduction is meaningful, it is an incomplete and often misleading representation of recovery.
Chiropractors encounter this disconnect daily as patients report less pain while continuing to demonstrate limited tolerance to activity, altered movement patterns, balance deficits, or rapid recurrence when physical demands increase and simply with time.
This gap has real consequences for patient adherence, long-term outcomes, and how conservative care is perceived within the broader healthcare system (i.e., conservative outcomes versus surgical) in terms of both cost and success.
Limits of Pain as a Primary Outcome
Pain is influenced by far more than tissue status alone. Central sensitization, psychosocial stress, sleep quality, expectation, duration, and prior injury history all shape symptom reporting. As a result, pain intensity correlates poorly with tissue health, functional capacity, and long-term disability, particularly in chronic and recurrent musculoskeletal conditions.1-2 Patients may experience short-term symptom relief while the underlying capacity of tissues and movement systems remain unchanged.
When pain is treated as the primary or sole outcome, care is often discontinued prematurely. This contributes to recurrence and reinforces the perception that conservative care offers temporary relief rather than durable recovery.
Attrition data from outpatient musculoskeletal rehabilitation supports this concern. Large observational and systematic studies consistently demonstrate that fewer than half of patients complete prescribed rehabilitation programs, with dropout frequently associated with early symptom change, pain during treatment and perceived lack of meaningful progress.3-5 These findings suggest pain-focused models fail to sustain engagement through the stages of recovery.
Pain-only framing does not simply limit measurement; it actively undermines adherence.
Why Pain Still Matters – But Cannot Be the Endpoint
Pain is not a distraction from care; it is the doorway into it. Patients seek chiropractic care because something hurts, and that pain must be addressed early and directly. Effective pain reduction reduces threat, restores a sense of safety and allows patients to re-engage with movement. In early care, pain modulation is not optional; it is essential.
However, population-level data consistently show that pain is rarely the true source of patient concern. Global Burden of Disease analyses demonstrate that musculoskeletal conditions are among the leading causes of years lived with disability, driven primarily by limitations in function rather than pain severity alone.6 Functional restriction is also a stronger predictor of healthcare utilization, work absence and long-term outcomes than pain intensity.7-8
In other words, patients may present with pain, but what they fear losing is function.
Pain can improve rapidly, often before tissue capacity, confidence and resilience are restored. When care remains focused exclusively on symptom reduction beyond this point, it fails to address the drivers of disability. This is where recurrence originates: not because pain was ignored, but because recovery was incomplete.
Pain is an early metric. Performance defines recovery.
Outcome Metrics Must Evolve With Phases of Care
A more effective approach aligns outcome measures with the biological and functional phases of healing. Early in care, pain intensity and symptom variability are appropriate markers of progress. They reflect reduced irritability and allow movement initiation.
As tissue health improves, outcome metrics must shift toward capacity. Tolerance to activity, recovery time following load, and functional endurance provide more meaningful insight into whether healing is occurring. A patient who can walk farther, stand longer or recover more quickly after physical demands is demonstrating objective improvement, even if some pain persists.
In later phases of care, performance-based outcomes become essential. Movement quality, symmetry, confidence, and readiness to return to work or sport determine whether gains will hold. When these metrics are ignored, recurrence becomes predictable rather than surprising.
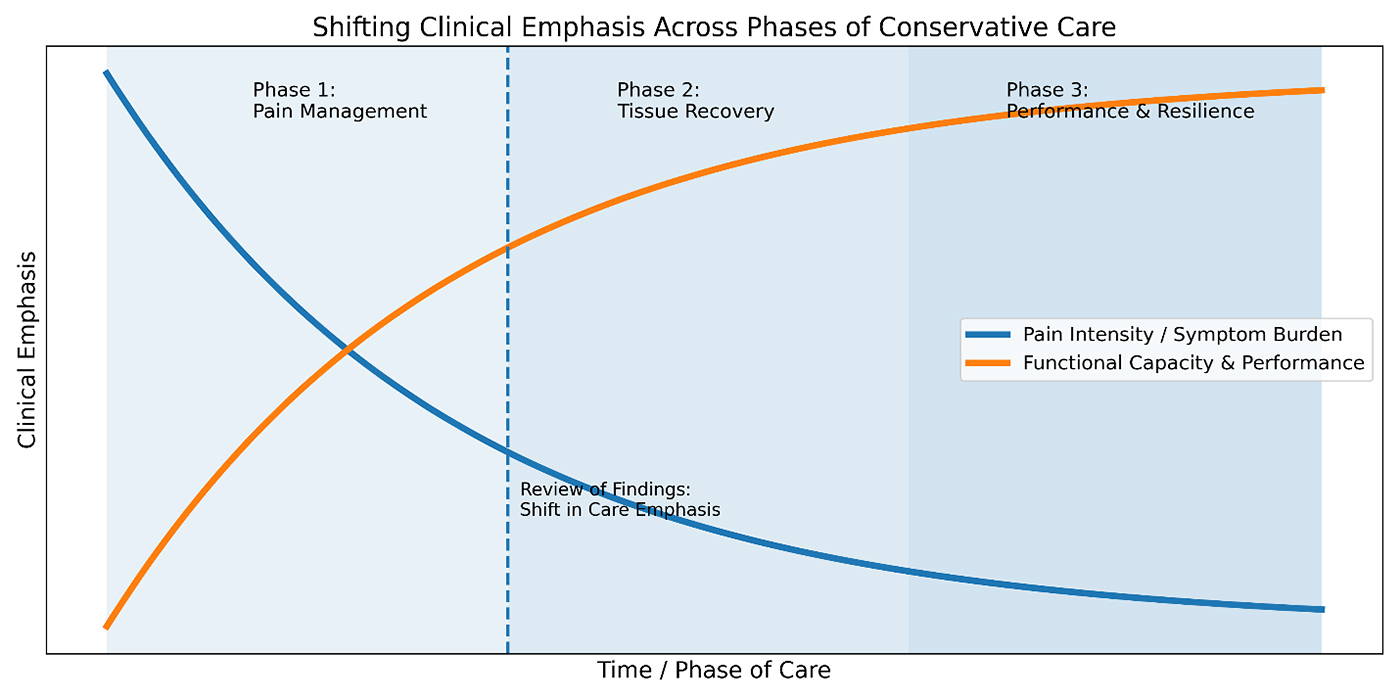
The ROF as a Turning Point
The review of findings is where chiropractors convert pain into purpose. It is the moment to shift the patient’s understanding from “why it hurts” to “what is limiting recovery.” When pain is contextualized within functional findings such as load intolerance, balance deficits, altered movement patterns, or delayed recovery following activity, care becomes outcome-driven rather than symptom-driven.
This conversation does not minimize pain. It explains its role. Pain becomes one signal within a broader recovery process rather than the sole determinant of success. When patients understand that reduced pain does not automatically mean restored capacity, adherence improves and premature discharge declines.
Why DCs Add System-Level Value
Conservative, function-focused care is associated with reduced imaging, lower opioid exposure, and delayed or avoided surgical intervention.9 Chiropractors add the greatest value when they intervene early, guide patients through recovery rather than symptom suppression, and reduce downstream healthcare burden.
By measuring performance and not just pain, chiropractors align with value-based care models while delivering outcomes patients actually care about.
Pain may open the door to care, but performance determines whether patients stay well. When patients have this understanding they may be more likely to return for maintenance sooner, before pain is the underlying deciding factor and further along in the injury cycle for any condition.
References
- Woolf CJ. Central sensitization: implications for the diagnosis and treatment of pain. Pain, 2011;152(3 Suppl):S2-S15.
- Hancock MJ, Maher CG, Laslett M, et al. What happened to the “bio” in the bio-psycho-social model of low back pain? Eur Spine J, 2011;20(12):2105-2110.
- Peek K, Sanson-Fisher R, Mackenzie L, Carey M. Interventions to aid patient adherence to physiotherapist-prescribed self-management strategies: a systematic review. Phys Ther, 2016;96(5):622-635.
- Hall AM, Ferreira PH, Maher CG, et al. The influence of the therapist–patient relationship on treatment outcome in physical rehabilitation: a systematic review. Phys Ther, 2010;90(8):1099-1110.
- Shahidi B, Padwal J, Lee E, et al. Factors impacting adherence to an exercise-based physical therapy program for individuals with low back pain. PLoS One, 2022;17(10):e0276326.
- Vos T, et al. Global burden of 369 diseases and injuries, 1990-2019. Lancet, 2020;396(10258):1204-1222.
- Park S, Stimpson JP, Fendrick AM. Health care utilization patterns among adults with or without functional disabilities. JAMA Netw Open, 2025;8(4):e254729.
- Hartvigsen J, et al. What low back pain is and why we need to pay attention. Lancet, 2018;391(10137):2356-2367.
- Whedon JM, Uptmor S, Toler AWJ, et al. Association between chiropractic care and use of prescription opioids among older medicare beneficiaries with spinal pain: a retrospective observational study. Chiropr Man Therap, 2022;30(1):5.



