A historic meeting between chiropractic and Make America Healthy Again (MAHA) leadership took place on March 10th, 2026, in Washington, D.C., featuring representatives from chiropractic national organizations, professional associations and policy principals. The collective goal: advancing the role of chiropractic in improving the health of Americans. Meeting participants focused on long-standing issues that have affected the chiropractic profession for decades, including access to care, reimbursement parity, and ensuring DCs have an appropriate role in national health policy discussions.
| Digital ExclusiveAntibiotics = Childhood Asthma?
A new study just published in the Journal of Clinical and Experimental Allergy has added fuel to the concern over the indiscriminate use of antibiotics.1 It has also begun to address the recent concern of scientists about the increasing occurrence of asthma in the United States.
The researchers surveyed parents of grade-school age children attending the Rudolf Steiner schools in New Zealand. These six schools were chosen because the schools' philosophy of illness causes it to "include a significant portion of parents who have rejected the use of conventional treatments, including antibiotics."
A survey was sent to the parents of 612 students, of which 456 (75%) were completed and returned. The survey was based on questions from the International Study on Asthma and Allergies in Children (ISAAC).
The history of the children revealed:
Antibiotic Use (ever) 74.7%
Antibiotic Use 36.3% (first year of life)
Any Vaccinations 75.5%
Ever Had Asthma 15.8%
The study looked at the odds ratio (risk) of children experiencing asthma symptoms based upon if, when, and how often they had taken antibiotics. The most decisive factors were when (before or after the first year of life) and how often. The results are quite sobering:
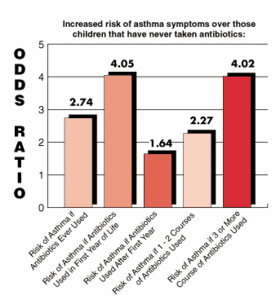
An "odds ratio" of 1.0 means the likelihood of a particular event occurring is equivalent whether or not a child has taken antibiotics. Thus, a child given antibiotics during the first year of life has an odds ratio of 4.05, which means the child is over four times more likely to develop asthma symptons than the child who has never taken antibiotics.
All of these odds ratios are adjusted for confounding factors of gender, ethnicity, family size, family history of asthma and parents' smoking habits. Without accounting for the confounders, the odds ratios are as much as six times the risk experienced by children who have never taken antibiotics.
So, now childhood asthma is added to the list of potential hazards to taking antibiotics.
This, along with the increase in antibiotic resistance, should cause patients to think twice about taking antibiotics, particularly where not specifically required.
Parents (and future parents) should be immediately made aware of this potential risk.
Julian Crane, associate professor at Otago University and one of the study's investigators, adds a note of caution about the findings: "Our paper, together with a study published last year in Thorax (Farooqi IS, et al. Thorax 1998;53:927-32), raises the possibility that broad-spectrum antibiotics, particularly in the first year of life, may be associated with an increased risk of atopy and asthma. For reasons that have been pointed out in both papers, these results cannot be taken as definitive, but rather as hypothesis-raising.
"On the other hand, the results are plausible. Broad-spectrum antibiotics came into clinical usage in the 1960s, and their increased use coincides with the time trends for the increasing prevalence of asthma. There is a plausible mechanism, namely that broad-spectrum antibiotics may alter and reduce bowel flora and thus switch off the immunological signals that these gut bacteria send to the developing immune system.
"Much more work needs to be done to check out whether this effect is causal, and if so, what are the immunological processess that cause it," professor Crane concluded.
Reference
1. Wickens K, Pearce N, Crane J, Beasley R. Antibiotic use in early childhood and the development of asthma. Clin Exp Allergy 1999;29:766-771.



